Tandem Diabetes Care insulin pumps are now powered by Control-IQ+ technology — the only predictive algorithm with AutoBolus, so you can start seeing improvements on Day 1.1
Automation for Tighter Control
Helps Prevent Highs
Control-IQ+ technology increases basal insulin dosing and uses AutoBolus (up to one an hour) if sensor glucose is predicted to be high.*
Helps Prevent Lows
Control-IQ+ technology can decrease or stop basal insulin if sensor glucose is predicted to be low. This can help improve time in range overnight and during the day.
Our Best Algorithm Ever
Now Available for Ages 2+
Expanded age and weight indications for very small and very large insulin requirements.
Temp Basal Rate
Temp Basal Rate option to personalize insulin delivery for changing needs during automation.
Extended Bolus
The only system with an extended bolus, up to eight hours, during automated insulin delivery.

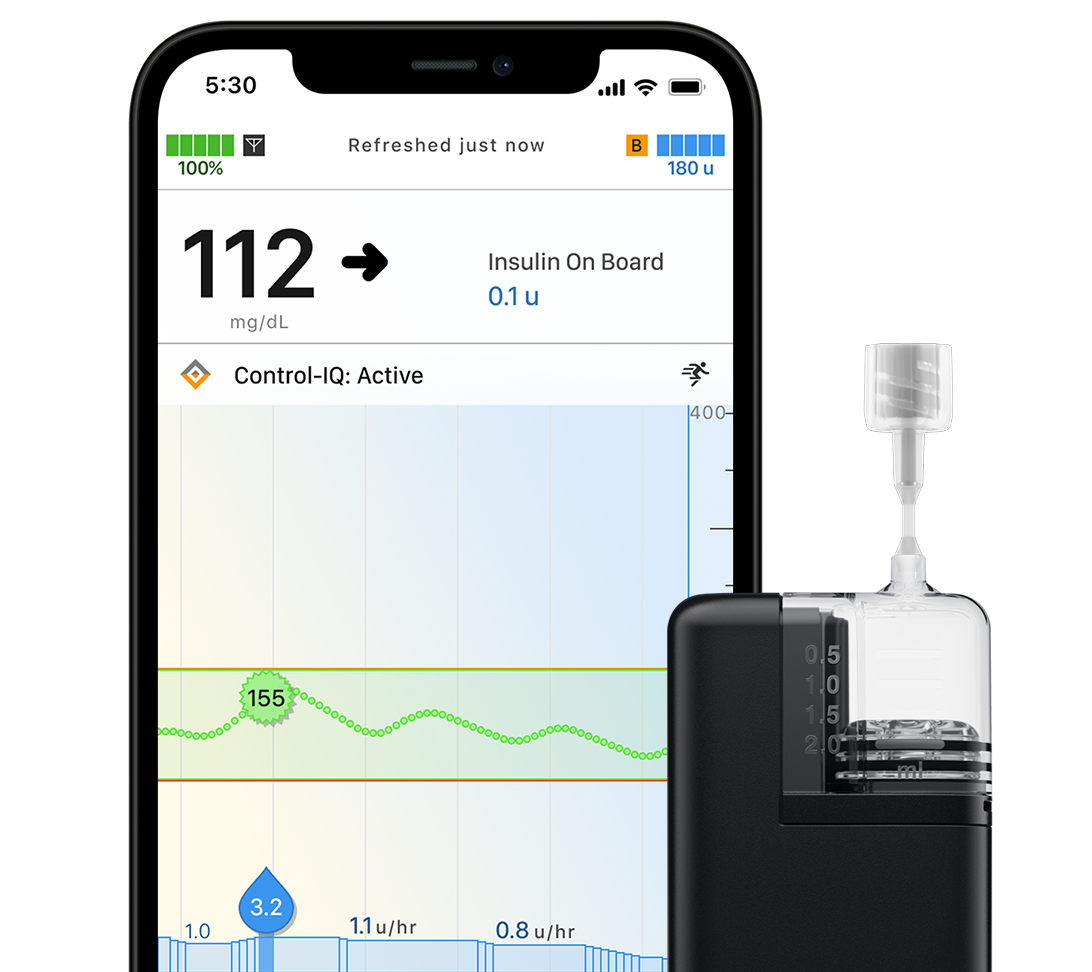
Control-IQ+ Technology The only system with AutoBolus
Only Control-IQ+ has a true automatic correction bolus.* If glucose is predicted to be above 180 mg/dL, an AutoBolus will be delivered.
Control-IQ+ with AutoBolus has demonstrated better A1c results, even for people who occasionally miss meal boluses.2

Best-in-Class Outcomes
Proven results with Tandem Diabetes Care automated insulin delivery systems.

Average Time in Range Increase on Day 11

Time in Range3†

Overnight Time in Range1

Reduction in A1c (Even if you rarely bolus!)2
Additional Activity Settings
Control-IQ+ technology includes optional activity settings that adjust the range of treatment values.
Sleep Activity
Uses a narrower and lower range of treatment values to help guard against lows and highs while sleeping.
Exercise Activity
Uses a narrower and higher range of treatment values to help guard against lows during activity.

Which Tandem insulin pump is right for you?
Whether you want the tiny and powerful Tandem Mobi system, or the all-in-one t:slim X2 pump, you can choose the automated insulin delivery system to fit your lifestyle. Which pump best fits you?

Order a Tandem Diabetes Care Automated Insulin Delivery System Today.
A Tandem Diabetes Care Specialist will help you get started.
Testimonials
See what people are saying about the Tandem automated insulin delivery and how it is changing their lives.
Read StoriesInfusion Sets
Choose from a variety of cannula materials, tubing lengths, and insertion angles to fit your needs.
Innovative Tools
Our mobile and cloud-based applications are designed to help you better manage your diabetes.
What's next?
Whether you're ready to get a Tandem insulin pump, or looking to check insurance coverage, you’ll find everything you need here.

